SDOH: How Does Access to NEMT Affect ER Diversion and Utilization? Part I
Last month, our Director of Social Determinants of Health (SDoH) and Product Development Tamara Carlton discussed how lack of reliable transportation to work programs, training programs, and more can affect individuals as they search for employment, ultimately leading to negative health outcomes. This month, she’s exploring the correlation between transportation and emergency care–specifically, how transportation as an SDoH can affect emergency care utilization and ER diversion.
ER Diversion: What Does it Mean?
The goal of ER diversion is to reduce low acuity and unnecessary ER visits. Unnecessary and expensive visits to the ER tie up medical resources needed for true emergencies, causing ER overcrowding and increasing the cost of medical care. One of the main causes of ER and EMS misuse? Lack of reliable transportation to primary care doctors for routine medical care, causing individuals to utilize EMS transportation to go to the ER instead. In a recent study by Emergency Physicians Monthly, approximately one quarter of ER patients arrive by EMS transportation, and less than half of those patients are actually admitted to the hospital. Not only are a very small number of EMS patients admitted, but the cost of the admissions is quite devastating for the hospital. On average, every 10 patients diverted costs the hospital four admissions, or roughly $24,000.
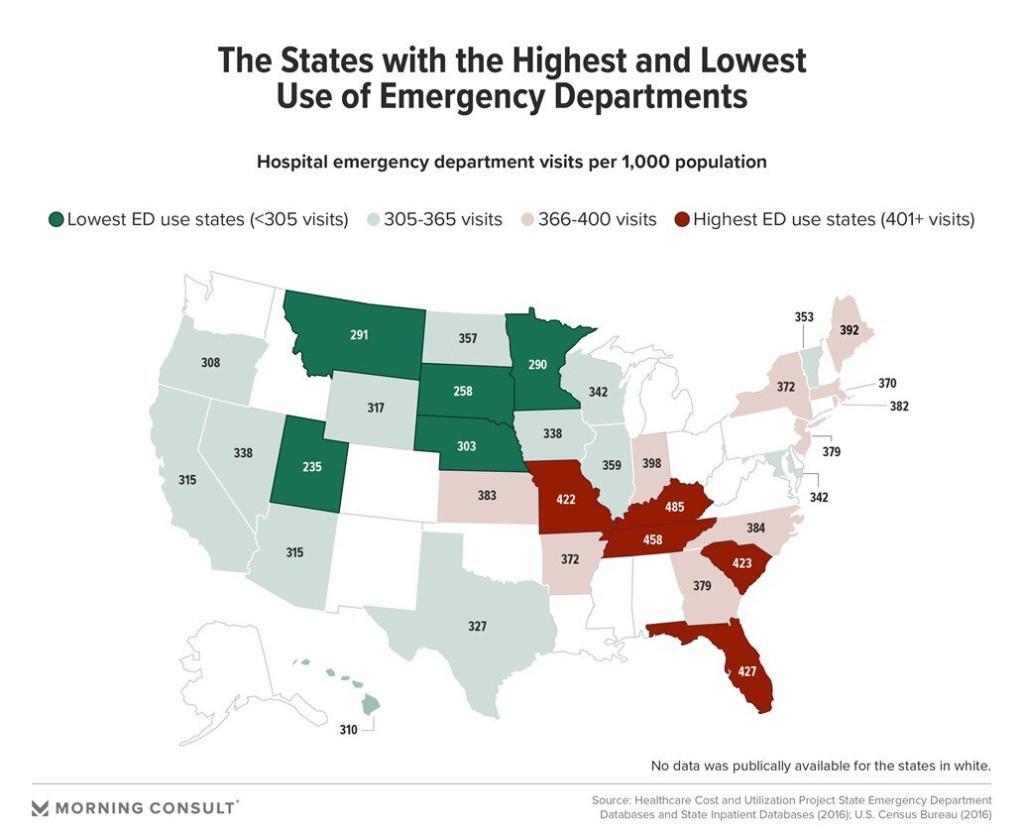
Further, Morning Consult, a global data intelligence company delivering insights to market research, conducted a recent study that found a strong relationship between emergency department visits at the state level and SDoH indicators, highlighting the states with the highest and lowest ER usage.
While social and economic factors can prevent people from accessing care, without accessible transportation to primary and preventative care appointments or non-emergency medical appointments like pharmacy trips, many patients have no other choice but to rely solely on emergency care options. Filtering into ERs, EMS transportation usage has seen a continued rise over the last five years, causing increased medical cost, higher premiums, and ER overflow nationwide. Dr. Greg Friese, MS, NRP, strongly advises his patients to not use 9-1-1 or other ambulance services. He says, “an ambulance is an expensive and economically inefficient mode of transport for many patients, especially those who don’t require lifesaving emergency care.”
How Does Access to NEMT Services Impact ER Diversion?
In addition to preventative care, non-emergent patients who need discharge, roundtrip dialysis, or rehab center transport are all examples in which Dr. Friese suggests using alternate transportation options, including non-emergency medical transportation (NEMT) when appropriate.
Access to NEMT services helps minimize the gap between members and access to healthcare – a key SDoH. Using NEMT to ensure members get to their medical appointments can allow ERs to create more space and give specialized care to patients who truly need it.
Tune in later this month to hear more about ER diversion and how it affects rural areas!
Categories
- Alaina Macia (39)
- Employee Wellness (19)
- ETO Newsletter (64)
- Events (70)
- MTM Health eNewsletter (83)
- News & Events (713)
- Technology (2)
- Tradeshows (57)
- Uncategorized (17)
- Webinars (15)